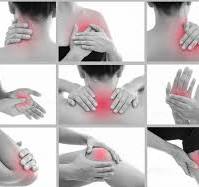
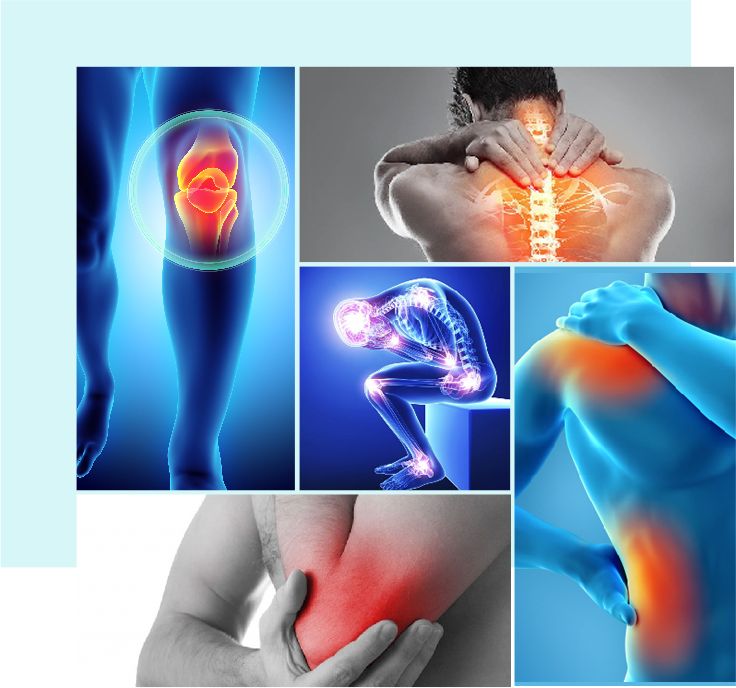
An experience of pain has several facets, including psychological, emotional, and physical aspects. It is a necessary physiological reaction meant to keep the body safe and promote recovery. Inflammation is a crucial factor in the development and maintenance of pain, both as a buffer against pain and as a possible cause of it. Understanding the complex link between inflammation and pain manage is essential to creating effective treatments and diagnosing a range of clinical problems.
Comprehending Inflammation
A complicated biological reaction to damaging stimuli like infections, damaged cells, or irritants is inflammation. It is a defense mechanism involving blood vessels, immunological cells, and molecular mediators. Eliminating the original source of cell harm, removing necrotic cells and tissues, and initiating a repair process are the main objectives of inflammation. Sustaining tissue homeostasis and general health depends on this process.Both acute and chronic inflammatory responses are possible. The body’s initial reaction to damage or infection is known as acute inflammation, and it is marked by redness, heat, swelling, discomfort, and loss of function. When the threat is eliminated, this kind of inflammation usually resolves and promotes healing. On the other hand, persistent inflammation results in tissue damage and is a contributing factor to a number of diseases, such as chronic pain disorders, cardiovascular diseases, and arthritis.
Mechanisms Connecting Pain and Inflammation
The primary mechanism by which inflammation and pain are linked is the activation of nociceptors, which are sensory neurons that transmit pain signals to the brain and spinal cord in response to potentially harmful stimuli. Numerous mediators, including prostaglandins, cytokines, and chemokines, are generated during inflammation. Peripheral sensitization is the process by which these drugs cause nociceptors to become more sensitive to stimuli by lowering their threshold.Lipid molecules called prostaglandins play a variety of physiological tasks, such as controlling pain and inflammation. They are produced by the cyclooxygenase (COX) enzyme from arachidonic acid. Prostaglandins intensify the pain response by making nociceptors more sensitive to other stimuli that cause pain.Tumor necrosis factor-alpha (TNF-α), chemokines, and interleukins (IL-1β, IL-6) are examples of cytokines that are important signaling proteins in the inflammatory process. They facilitate the release of more inflammatory mediators and encourage the migration of immune cells to the site of injury. Because they can cause hyperalgesia (heightened sensitivity to pain) by acting directly on nociceptors or by inducing the production of other pro-inflammatory agents, TNF-α and IL-1β are particularly important in the control of pain.The calcitonin gene-related peptide (CGRP) and substance P are two examples of neuropeptides that are implicated in the inflammation-pain pathway. These neuropeptides cause vasodilation and increase vascular permeability, which in turn contribute to the inflammatory response. They are released from the nerve endings of nociceptors. It is known that Substance P in particular increases the release of pro-inflammatory cytokines, which in turn improves perception of pain.
Chronic Pain and Inflammation
Millions of individuals throughout the world suffer greatly from chronic pain, a serious health problem that lowers their quality of life. In contrast to acute pain, which goes away when the underlying cause is addressed, chronic pain lasts for longer periods of time and has the potential to develop into a disease. A frequent underlying cause of many chronic pain problems is chronic inflammation.One of the best examples of a disorder in which chronic inflammation is essential to the onset and maintenance of pain is osteoarthritis (OA). Inflammatory mediators are released as cartilage breaks down in OA, activating nociceptors and causing ongoing discomfort. Cytokines including TNF-α and IL-1β are present in the inflammatory phase of OA and lead to pain sensitivity and cartilage deterioration.Another illness where chronic inflammation and pain are closely associated is rheumatoid arthritis (RA). An autoimmune condition called rheumatoid arthritis (RA) is defined by persistent joint inflammation, which can cause discomfort, edema, and ultimately joint degeneration. The intricate interaction between immune cells, cytokines, and autoantibodies that maintains the inflammatory response is what causes discomfort in people with RA.One kind of persistent pain that results from harm to the nerve system itself is called neuropathic pain. By further destroying nerve tissues and increasing pain pathway sensitivity, inflammation can worsen the pain in diseases like diabetic neuropathy and postherpetic neuralgia. The significance of managing inflammation in order to properly manage pain is highlighted by the function of inflammatory mediators in neuropathic pain.
Pain Relief Anti-Inflammatory Therapies
Anti-inflammatory medications are essential components of pain therapy because of the important role that inflammation plays in pain. NSAIDs, or nonsteroidal anti-inflammatory drugs, are among of the most widely prescribed treatments for pain relief. NSAIDs function by preventing the cyclooxygenase enzymes (COX-1 and COX-2), which lowers prostaglandin synthesis. Pain sensitivity and inflammation are reduced as a result. Prolonged NSAID use, however, can have negative side effects, such as increased risk of cardiovascular disease and gastrointestinal issues.Another type of anti-inflammatory medications that is very good in lowering pain and inflammation is corticosteroids. They function by reducing the synthesis of inflammatory mediators and inhibiting the immunological response. Although corticosteroids are frequently used to treat severe inflammatory diseases, their long-term use is constrained by possible adverse effects such osteoporosis and immunosuppression.Biologics are a more recent method of focusing on particular aspects of the inflammatory process. Examples of these include fusion proteins and monoclonal antibodies. In the case of rheumatoid arthritis, for example, TNF inhibitors like infliximab and adalimumab have demonstrated a notable effectiveness in lowering pain and inflammation. By selectively targeting TNF-α, a crucial cytokine in the inflammatory cascade, these biologic medicines effectively reduce pain and inflammation.Alternative therapy and lifestyle adjustments are important in the management of pain and inflammation. Exercise, stress reduction, and diet can all affect the inflammatory process. Systemic inflammation can be decreased by diets high in anti-inflammatory nutrients such phytochemicals, antioxidants, and omega-3 fatty acids. Frequent exercise has been demonstrated to reduce pain and offer anti-inflammatory properties, especially in disorders like osteoarthritis. Methods of reducing stress, such yoga and mindfulness, can also control the inflammatory response and enhance the results of pain.
In summary
Research on how inflammation affects pain is crucial because it has a big impact on how different types of pain are treated. Knowing how inflammation affects pain can help develop more specialized and efficient treatments. The relationship between inflammation and pain is intricate and multidimensional, ranging from the acute inflammatory response that sensitizes nociceptors to the chronic inflammation that prolongs pain in conditions like rheumatoid arthritis and osteoarthritis.The mainstay of pain management approaches is anti-inflammatory therapy, such as biologics, corticosteroids, and NSAIDs. To achieve the best pain relief, a balanced approach incorporating lifestyle changes and alternative therapies is necessary due to the possible adverse effects of these treatments. There remains potential for more individualized and efficient pain management strategies that target the underlying inflammatory processes as research into the complexities of the link between inflammation and pain continues.